The mission of the Institute for Child and Family Well-Being is to improve the lives of children and families with complex challenges by implementing effective programs, conducting cutting-edge research, engaging communities, and promoting systems change.
The Institute for Child and Family Well-Being is a collaboration between Children’s Wisconsin and the Helen Bader School of Social Welfare at the University of Wisconsin-Milwaukee. The shared values and strengths of this academic-community partnership are reflected in the Institute’s three core service areas: Program Design and Implementation, Research and Evaluation, and Community Engagement and Systems Change.
In This Issue
- Reflections on our 5th Anniversary as the ICFW
- Meet the ICFW Affiliates – Dr. Julian Ford, Clarence Johnson, & Dr. Christy Warner-Metzger
- ICFW Recognition
- Program Design and Implementation
- Research and Evaluation
- Community Engagement and Systems Change
- Recent and Upcoming Events
Reflections on Our 5th Anniversary
A Message from Our Co-Directors, Gabe McGaughey and Josh Mersky
This newsletter marks the fifth anniversary of the Institute for Child and Family Well-being. As we reflect on the past five years, we are humbled by the opportunities we have had to join many others who are dedicated to strengthening families and nurturing children. Our community-university partnership emerged from a shared commitment to promoting the well-being of all children and families and to addressing barriers that result in unequal access to the best available care. We do so by translating the science of what works into prevention and intervention strategies that are effective in the real world. Central to this process is the relationships that are present in communities, organizations, and systems with whom we work with to integrate effective, culturally responsive, and sustainable solutions. The list of agencies and stakeholders who deserve our gratitude is too long to acknowledge here, but we invite you to check out our project pages where you will find many of our key partners.
As we look to the future, our aim is to strengthen these alliances and forge new community connections that are necessary to disseminate effective strategies and produce lasting systems change. In that spirit, we will be organizing a series of events over the next year to support the exchanging of information, building relationships, and translating knowledge into action. We hosted our first event in April to highlight our Program Design and Implementation efforts with group-based, telehealth therapy. To learn more about upcoming events, follow us on social media, visit our website, and subscribe to our newsletter.
We hope that you will join us!
Meet the ICFW Affiliates
As Community Engagement and Systems Change are a core pillar of the ICFW, collaboration with our community and systems partners is critical to fulfilling our mission. In recognition of those that value collaboration and whose mission seeks to improve child and family well-being, we have invited those partners to join us as ICFW Affiliates. We are honored to introduce our three newest ICFW Affiliates with whom we look forward to partnering with now and into the future.

Dr. Julian Ford, Ph.D., A.B.P.P.
Dr. Ford is a board certified clinical psychologist and Professor of Psychiatry and Law at the University of Connecticut where he directs two Treatment and Services Adaptation Centers in the National Child Traumatic Stress Network: the Center for Trauma Recovery and Juvenile Justice and the Center for the Treatment of Developmental Trauma Disorders. Dr. Ford is past President of the International Society for Traumatic Stress Studies, and a Fellow of the American Psychological Association. He has published more than 250 articles and book chapters and is the author or editor of 10 books, including Posttraumatic Stress Disorder, 2nd Edition, Treating Complex Trauma: A Sequenced, Relationship-Based Approach, 2nd Edition, Treating Complex Traumatic Stress Disorders in Children and Adolescents: Scientific Foundations and Therapeutic Models, and Critical Moments: Transforming Crises into Turning Points in Psychotherapy. Dr. Ford is the Principal Investigator for the national Developmental Trauma Disorder Field trial research study, and developed and has conducted randomized clinical trial and effectiveness studies with the Trauma Affect Regulation: Guide for Education and Therapy (TARGET©) model for youths and adults with developmental trauma histories and complex PTSD.
ICFW leaders have collaborated with Dr. Julian Ford, an international leader in traumatic stress studies, on several occasions. First, Dr. Ford served as an expert consultant during initial implementation of the trauma screening, brief intervention, and referral to treatment (T-SBIRT) protocol. Subsequently, he co-authored the initial T-SBIRT feasibility study that Dr. Topitzes published in 2017 along with Dr. Mersky (Topitzes et al., 2017). Second, Dr. Ford presented his trauma counseling model for youth, TARGET, in a symposium led by Dr. Mersky at the Society for Social Work and Research 2018 annual conference. Dedicated to exploring new frontiers in trauma research, the symposium included presentations delivered by Drs. Mersky and Topitzes. Future collaborations might center on the continued development of the T-SBIRT and TARGET models.

Mr. Clarence Johnson is currently serving as the Executive Director of Wisconsin Community Services. The mission of WCS is to advocate for justice and community safety, providing innovative opportunities for individuals to overcome adversity. Mr. Johnson was instrumental in leading the effort that resulted in the WCS Center for Driver’s License Recovery being named as one of Mutual of America’s three national 2019 Community Partnership Award winners. Clarence also brought Community Building Milwaukee to WCS, which involves numerous agencies, institutions and organizations across the Milwaukee community serving, youth and adults.
Mr. Johnson believes the key ingredients to effective and successful leadership include holding yourself accountable to the highest standards of performance and empowering and supporting others to reach for their highest level of effectiveness. As one of the most experienced African American nonprofit leaders in the Milwaukee area, he has helped shape the future of several nonprofit organizations in the Milwaukee Community and is held in high regard in many circles. During his long and distinguished career, Mr. Johnson has served on over 20 nonprofit boards and remains an active member of the Milwaukee area community. He was recently elected to the board of directors of the Wisconsin Association of Family and Children’s agencies and also serves as a board member for NAMI Southeast Wisconsin.
Mr. Johnson is a lifelong resident of city of Milwaukee and earned both his undergraduate and graduate degree from the University of Wisconsin-Milwaukee. He has worked on several research projects during his career and began a program to reduce the incidence of obesity and chronic disease among central youth. Working for over 35 years in Social Services, Mr. Johnson has served as Executive Director of Neighborhood House of Milwaukee, Chief Operating Officer for YW Works, and as a high level manager for Milwaukee County Department of Health and Social Services.
ICFW leaders have worked directly with Mr. Johnson in several capacities. Dr. Topitzes, for instance, serves on the WCS board of directors and on several project-based work groups overseen by WCS and Mr. Johnson, including the Community Building Milwaukee Steering Committee.

Christina Warner-Metzger, Ph.D., hails from Oklahoma State University with a doctorate in Clinical Psychology. True to her organization’s motto of Doing good and doing it wellTM, Dr. Warner-Metzger founded Evidence-based Practices and International Consulting (EPIC), LLC, to promote increased accessibility and excellence in professional training, consultation, and program development within the mental health and wellness sector. With a focus on training culturally humble and socially responsible professionals, she also directs the Parent-Child Interaction Therapy (PCIT) Program and Early Assessment and Recommendations for Learning in Young Children (EARLY) Clinic at DePaul University’s Family and Community Services. She is 1 of 21 PCIT International Certified Global Trainers worldwide and a Child-Adult Relationship Enhancement (CARE) co-developer, which provides her with clinical expertise in PCIT and CARE training and dissemination. Dr. Warner-Metzger is also the co-developer of a project piloting Trauma-Directed Interaction (TDI) with young children. She has served as a trainer and consultant for dissemination efforts across the United States, as well as Indonesia and Australia. Her contributions as an expert trainer and consultant on institutional, regional, federal, and international grant-funded projects has spanned the greater part of the past decade.
She is also experienced using the National Child Traumatic Stress Network (NCTSN) Learning Collaborative model. Dr. Warner-Metzger’s clinical and research interests include Autism Spectrum Disorders (ASD), developmental disabilities, disruptive behavior disorders, trauma-informed systems, underserved populations, barriers to treatment participation, and dissemination efforts. She has contributed to these topics through numerous peer-reviewed and invited presentations at national and international conferences, as well as authored peer-reviewed journal articles, government publications, and edited book chapters. Her previous clinical work in Memphis and current work in Chicago has focused on serving urban populations experiencing economic and racial marginalization.
ICFW leaders and clinicians, Dimitri Topitzes, Kate Bennett, and Leah Cerwin have worked closely with Dr. Warner-Metzger in their continuing development as certified PCIT International Within-Agency and Regional Trainers as part of the Trauma & Recovery Project. Dr. Warner-Metzger has also co-facilitated PCIT Therapist Trainings with our team in Milwaukee and as part of a statewide dissemination project in Utah.
ICFW Recognition

Congratulations to Ross Gilbert on matching for his residency in Internal Medicine and Pediatrics at Johns Hopkins Medicine-Pediatrics Urban Health Residency Program in Baltimore, Maryland. Ross has worked with the ICFW as a fellow through the TRIUMPH program while completing medical school at UW-Madison.
Congratulations to Mary Kusch on her acceptance to the Wisconsin Population Health Service Fellowship Program. She will be placed with the Wisconsin Division of Public Health, Bureau of Environmental and Occupational Health. Mary has worked with the ICFW as a research assistant while completing her master’s degree at the UWM Zilber School of Public Health.
Program Design & Implementation
The Institute develops, implements and disseminates validated prevention and intervention strategies that are accessible in real-world settings.
Minecraft® to Build Our Children’s Social Skills
The Institute for Child and Family Well-Being consulted with Children’s Wisconsin professionals across the state to develop Community Services’ COVID Resilience Plan. During this process, a collaboration between Black River Falls Family Support Prevention Program and the ICFW resulted in a virtual, game-based social skill building group opening up to children statewide. This program is designed to help youth acquire social and communication skills to help them interact with others more successfully.
Minecraft® and the work of Australian psychologist Raelene Dundon are used by a Family Support Specialist in secure video teleconferencing software currently in a 1:1 format. This will be the first iteration of using groups and inviting children from all over Wisconsin. The program will target the improvement of social and emotional skills such as social communication, cooperation, problem solving, and self-control. Weekly touch points with caregivers and the use of the Manatee app will help monitor goals and foster communication between the provider and caregivers. Our Before Action Review was used to help create workflows, determine how to collect data and set goals. An After Action Review will be used to log design learning, propose improvements and assess for possible scalability. In future iterations, data will be gathered on executive functioning pre and post completion to examine possible correlations between participation in group and improved functioning.
If you would like more information on referring a child, please email mchristian@chw.org.
Learn More:
ICFW Practice Brief – After Action Reviews (PDF)
ICFW Practice Brief – Strategic Learning (PDF)
Raelene Dundon
Parenting with P.R.I.D.E. and Web-based Assessments
By Kate Bennett
As the ICFW clinical team continues to work toward improved iterations of group-based intervention modifications, we are reminded that successful program design and implementation relies on collecting and analyzing quality data. While data is critical for program analysis, it is also one of the cornerstones of Parent-Child Interaction Therapy (PCIT) treatment and the multifamily Parenting with P.R.I.D.E. intervention.
The screening and assessment tools typically applied in PCIT are accessible for use at Children’s Wisconsin and include the following:
- Eyberg Child Behavior Inventory (ECBI; Eyberg & Pincus, 1999)
- Child Behavior Checklist for ages 1.5-5 and ages 6-18 (CBCL; Achenbach & Rescorla, 2001)
- Dyadic Parent–Child Interaction Coding System, Fourth Edition (DPICS‑IV; Eyberg et al., 2013)
- Parenting Stress Index, Fourth Edition: Short Form (PSI‑4: SF; Abidin, 2012).

Because the ongoing administration and analysis of each of these assessments results are critical to individual patient/family treatment and the overall program evaluation, our clinicians have been piloting the use of web-based assessment forms. Our purpose in moving to electronic administration and scoring is to enhance convenience for both clinicians and families as we continue forward with telehealth delivery of Parenting with P.R.I.D.E. and other trauma-based treatment groups. For example, web-based administration of the ECBI through Psychological Assessment Resources allows a parent/caregiver to report on child behavioral observations on a weekly basis from their phone or laptop throughout the duration of treatment. Form completion takes approximately 5 minutes for a respondent and is entered within 24 hours prior to the family checking into a therapy session. The assigned clinician receives the assessment results in real-time. This allows for more focused time in treatment, and additionally contributes to the fidelity of goal-directed services for families.
Our intention is to continue to pilot the use of web-based screening and assessment tools for ease of caregiver completion, immediate scoring, and automatic skill progress tracking throughout treatment for PCIT and other evidence-based treatments. We look forward to sharing our findings and feedback from families in coming newsletters and reports.
References:
- Abidin, R. R. (2012). Parenting stress index–fourth edition (PSI-4). Lutz, FL: Psychological Assessment Resources.
- Achenbach, T.M., & Rescorla, L.A. (2001). Manual for the ASEBA School-Age Forms & Profiles. Burlington, VT: University of Vermont, Research Center for Children, Youth, & Families.
- Eyberg, S., & Pincus, D. (1999). Eyberg child behavior inventory & Sutter-Eyberg student behavior inventory-revised: Professional manual. Psychological Assessment Resources.
- Eyberg, S. M., Nelson, M. M., Ginn, N. C., Bhuiyan, N., & Boggs, S. R. (2013). Dyadic parent–child interaction coding system, 4th edition (DPICS-IV) comprehensive manual for research and training. Gainesville, FL: PCIT International.
Learn More:
Psychological Assessment Resources
Achenbach System of Empirically Based Assessment
PCIT International
Research and Evaluation
The Institute accelerates the process of translating knowledge into direct practices, programs and policies that promote health and well-being, and provides analytic, data management and grant-writing support.
Milwaukee Equity Action Plan
Leaders at the Institute for Child and Family Well-Being at UWM are collaborating with the Wisconsin Department of Workforce Development, Division of Vocational Rehabilitation (DVR) to develop, implement and test a consumer quality improvement plan at the Milwaukee central city location. This initiative builds on an extensive consumer service review that DVR conducted in 2019. Stakeholder interviews revealed that Milwaukee-area DVR consumers, the majority of whom are Black Americans, face multiple barriers to effective service engagement and completion. These include extreme poverty resulting from structural racism, significant distress due to current and historical trauma, and poor service access owing to organizational policies and procedures. Titled the Milwaukee Equity Action Plan, the consumer quality improvement plan aims to enhance the culturally responsive and trauma-informed nature of DVR consumer services.
Members of the Institute’s team for the Milwaukee Equity Action Plan project will help translate insights from the field and results from DVR’s consumer service review into a viable quality improvement plan. The Institute team will also develop and execute an evaluation plan to help DVR gauge progress toward consumer service goals and adjust the quality improvement plan as needed. In addition, the team will help DVR develop a sustainable, high quality consumer service model that reflects its values.
Learn More:
Recent ICFW Publications
Practice Brief: COVID Resilience Plan for Nonprofits (PDF)
The Impact of the COVID-19 Pandemic on Maternal Mental Health – Meghan Majors from the 2021 (virtual) UWM Health Research Symposium.
Community Engagement & Systems Change
The Institute develops community-university partnerships to promote systems change that increases the accessibility of evidence-based and evidence-informed practices.
Seeking Solutions for Youth Aging Out of Foster Care
By Luke Waldo
In November 2020, Children’s Wisconsin’s and collaborating partners, Wisconsin Department of Children and Families and Bay Area Workforce Development Board, began working on a planning grant to facilitate a community assessment to determine the causes of poor outcomes for youth between the ages of 18-24 who are aging out of foster care and to propose targeted solutions. The assessment surveyed the region’s strengths, resources, needs and gaps as they relate to the population of youth transitioning to adulthood in Northeastern Wisconsin.
Through these collective efforts, the long-term goal is to provide a pathway to independence by strengthening youths’ resiliency and equipping them with the knowledge and skills necessary to become self-sufficient, build a strong support network, achieve educational and/or job training goals to earn a living wage, and maintain safe and stable housing.
Over four months, insights were gathered from leaders, staff and administrators working within the region’s Independent Living systems, as well as from youth and young adults who have received services through those systems. We used a human-centered design approach in the development of the assessment. A core planning team consisting of representatives from the following organizations and groups developed the assessment:
- Wisconsin Department of Children and Families – Independent Living Program
- Bay Area Workforce Development Board – Region II Independent Living Service Providers
- Youth Advisory Council – Youth who have been involved with child welfare systems
Data were collected through surveys, focus groups and literature review.
Surveys
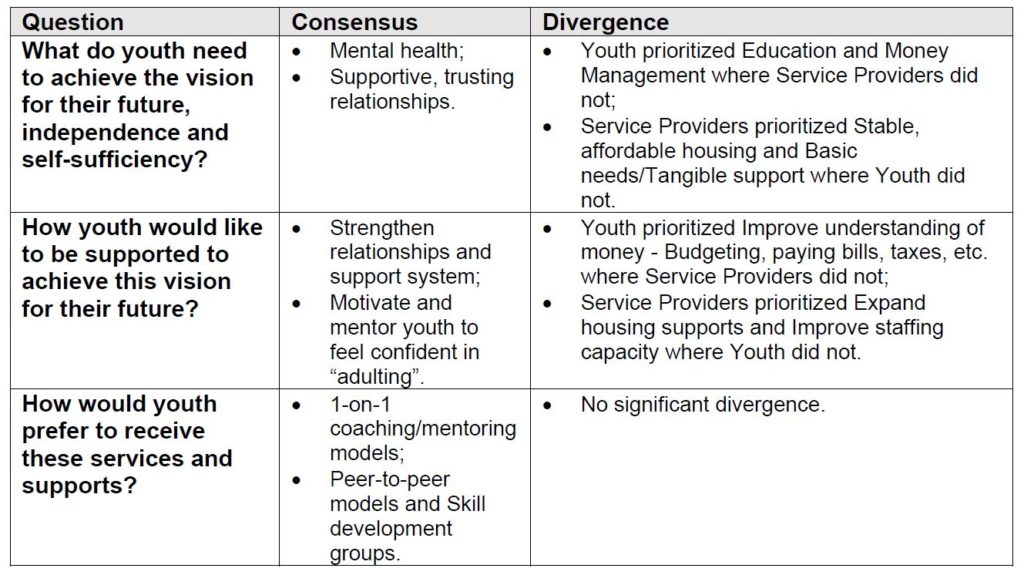
Between the youth/young adult and provider surveys, there were areas of strong consensus and divergence in the responses noted in Table 1. Consensus occurred when youth and provider responses had strong consensus within and across groups. Divergence occurred when strong consensus was present in one of the surveyed groups but not the other.
Table 1:
Focus Groups
Focus Groups were conducted over 90 minutes on Zoom due to COVID-19 safety and health requirements. Participants were asked a series of questions and were provided between 1-3 minutes to individually reply in the Chat box. Upon completing individual brainstorming, the facilitators identified themes and asked participants to elaborate on those themes and ideas. Between the youth/young adult and provider focus groups, there were areas of strong consensus and divergence noted in Table 2.
Table 2:

Lessons Learned: The Importance of Mental Health and Supportive Relationships
During our assessment, we came back to a number of key questions for youth and providers in response to the prioritization of mental health. Do youth today have more mental health needs, or are we just more aware of those needs? Are housing and financial stability less important to youth today, or do youth prioritize them lower than mental health in recognition that they are much more difficult to obtain and maintain when they are struggling with mental health issues?
While elaborating on why mental health is a bigger concern than it may have been in the past, one of our youth team members said that managing overwhelming feelings and stress is harder to manage than the initial cause of the stress (i.e. relationship or financial issues). She expressed that there might be a generation gap as it was not previously “acceptable” to talk about mental health.
Throughout this assessment, we have heard how having a trusted, supportive person to talk to, even if they aren’t a mental health professional, can be beneficial in strengthening youth’s executive functioning (i.e. enhancing coping and organizational skills). Ultimately, we see potential for meaningful impact by training service providers in trauma, mental health and strengths-based engagement so that they may support youth’s mental well-being and executive functioning, while not expecting them to serve as mental health professionals for youth.
During the final phase of this planning grant, we will develop and identify solutions that align with the lessons learned from the regional assessment. Our final analysis and proposed solutions will be delivered to the regional funder, Oshkosh Area Community Foundation, and the grant partners for future funding and implementation consideration.
Children’s Mental Health in Times of COVID: Interviews with ICFW Clinicians
By ICFW Interns – Paige Bintz, Kelah Hatcher, and Johanna Nelson (photos in order)



While the ICFW clinicians were adapting their therapy to virtual platforms in response to the COVID crisis, the need for Parent-Child Interaction Therapy (PCIT) was growing. From the end of in-person visits until the start of virtual therapy in May, a significant waitlist had developed. The stress related to COVID-19 seemed to have created and exacerbated mental health issues for children and their families.
Early on in virtual therapy, clinicians noticed an increase in externalizing behaviors for both caregivers and children. Irritability, animosity, and jealousy towards siblings were some of the commonly reported behaviors that clinicians saw in response to children adjusting to COVID-19. Family relationships also were impacted due to increased time spent together while kids were doing school virtually and caregivers worked from home or had lost their jobs. Consequently, caregivers reported more conflicts with their children and between siblings.
Several months into the pandemic, the clinicians began hearing caregivers attributing their children’s challenges directly to the impact of COVID-19. Our clinicians noted an increase in internalizing behavior such as fatigue, anxiety, and depression in children. Symptoms of social anxiety or anxiety around getting sick were also reported more often than previously.
The effect of the pandemic on children’s school experience has varied based on numerous factors. Younger children have struggled more with remaining attentive during virtual learning, while older children have suffered from the lack of social interaction with their peers. For families with multiple children, a lack of consistency between virtual and in-person learning for different age groups has also presented a challenge. However, children are more resilient than we often realize, and the support provided by their families and teachers can make a big difference.
Children of all ages had to adjust to virtual learning and then back to hybrid or fully in-person learning. Virtual learning is unfortunately less cooperative, and older students have shared that they have been stressed by an increase in assignments. More students than usual are “behind”, and while eager to see their friends and teachers, they may not want to return to in-person school if it’s not the same as before. It’s difficult to predict if there will be a long-term impact on social skills, especially for younger children, but so far there is no indication of that. Conversely, a lack of closure for older students, especially seniors, has been disappointing, but again their experience was often dependent on how their school supported them.
The clinicians are noticing that the grief process has been intense for children and families who have experienced loss (i.e. death of a family member, employment, normalcy with school, social life, etc.). They are having to identify loss and know what it looks like, which can be difficult without social interaction. Without social situations due to the pandemic, children are having a harder time developing empathy and different point of views which is strengthened through interaction. Children are being siloed into basic emotional words but grief is a continuous cycle that is more complex than “sad” or “mad”. Caregivers can have difficulty with this too. With a noticeable increase in parental stress, there may be “shorter fuses”. Caregivers are going into survival mode, trying to keep their children safe from disease as well as maintain the mental and economic well-being of their family. Clinicians are noticing that parental response to children’s grief along with their own is key to process the past year and build emotional awareness.
All of this stress and grief seems to have reached an equilibrium due to telehealth, according to the clinicians. Mental health services have become more accessible with the push to virtual formats. Clients do not need to worry about childcare, transportation, or other barriers when seeing their care provider from the comfort of their own home. Families are more willing to reach out for help online. Because of this, clinicians push for more agency leaders, insurance companies, and other services to keep telehealth options and increase accessibility for families in need post pandemic. This way caregivers can focus on the relationships they build with their children, managing emotions and behaviors, responding to uncertainty, and building resilience.
The ICFW Clinicians’ Tips to Building Resilience:
- Acknowledge the gravity and complexity of this past year
Encouraging emotional labeling with children is key to helping them understand what the pandemic is and how it has impacted them. Then focus on validation. Let the children know that this has an impact on everyone and they are not alone.
- Set up a conversation on boundaries and needs
Come together as a family and determine what boundaries need to be implemented in order to maintain emotional and physical well-being. Saying “no” can be difficult, but caregivers should emphasize self-care and what is best for the family. An example of a boundary could include electronic use because of the increased need for virtual access during the pandemic. Now may be a good time to develop a plan to return to basics or having conversations about healthy electronic use with children.
- Be mindful in reintroducing social situations
At this point of the pandemic, people are exhausted and social interaction can be overwhelming. To minimize the stress of this, set up a hierarchy of social stimulation and work your way upwards with the child. For example, this means starting with a walk around the block and working your way up to sitting in a classroom surrounded by other children. Overall, be proactive about creating a safe place and work in short bursts to make the transition smoother.
- Build a sense of routine
Caregivers should be mindful of preparing children for possible unknowns, but having a daily routine is key to dealing with tough situations like a pandemic. Caregivers could plan out the day and create visual charts, that way the children can tangibly see and check off accomplishments during the day. Make sure to praise for any adaptation that the child is going through and say that you are proud they are dealing with difficulty. Also, building the routine may be a great opportunity to set new and healthier habits that get back to family time.
Recent and Upcoming Events
The Institute provides training, consultation and technical assistance to help human service agencies implement and replicate best practices. If you are interested in training or technical assistance, please complete our speaker request form.
ICFW 5th Anniversary – May 2021
Schedule of events to celebrate our anniversary year and highlight our efforts to achieve our mission will be announced soon on our website and social media.
ICFW Webinars:
April:
Presentations, Trainings and Workshops:
April:
Together for Children Conference: Vicarious Trauma: Honoring the Weight of our Work – Meghan Christian and Luke Waldo
Together for Children Conference: Asking Sensitive Questions: Effectively Assessing for Exposure to Trauma and Adversity – Kate Bennett and Dimitri Topitzes
May and July 2021:

