Why Does Family Engagement Matter?
Home visiting programs provide support and services to enhance the health and well-being of children and their caregivers, particularly in vulnerable and economically disadvantaged populations. Research indicates that home visiting services can promote maternal and child health, nurturing home environments, and gains in child development.1
But success hinges on the extent to which families engage in services. Most evidence-based programs make services available to families for multiple years, but the majority of clients receive services for a year or less.2 Compounding this problem, the families who may benefit most from home visiting are also the ones who may be hardest to reach, enroll, and retain. Moreover, evidence from home visiting and other service sectors suggests that participation alone is a poor predictor of client outcomes.3
One reason this might be the case is that there is a difference between program participation and engagement: Participation refers to signs of client and program activity, such as enrollment, number and frequency of visits, and service completion. Engagement reflects the quality of client attitudes toward, emotional investment in, and behaviors related to their services and service providers.4
It may be that participation is a necessary but not sufficient condition for success. This issue brief presents what we know about participation and engagement based on the available literature and new findings from Wisconsin’s Family Foundation Home Visiting (FFHV) program.
Initiating Program Participation
For many programs, outreach periods can last several weeks and even months. Most families that accept services, however, do so within a shorter period of time. For families that accepted services from one of Wisconsin’s FFHV programs since January 2015, the median time spent in recruitment was 15 days. Over three-fourths (77%) of families that received services enrolled within the first 30 days of outreach.
Many potential clients decline voluntary services because they feel they do not need them. Results from the FFHV evaluation indicate that over half (56%) of individuals who declined to enroll reported they did not need services or they already had adequate support. Yet, programs often do not receive a definitive answer from clients regarding their intent to enroll in or decline services. Programs may find that “passive” refusals are more common than active refusals. A passive refusal is when a client agrees to services but is never available for a visit. One review of Healthy Families America (HFA) programs reported that only 5-10% of clients refused services outright, but 20-30% of individuals that accepted services did not complete a single visit.5
Sustaining Program Participation
Although guidelines for optimal service duration vary, many program models recommend that families receive services for multiple years. However, studies consistently show that a large majority do not receive services for that long.
On the other hand, the expected length of service according to model standards may not be a good gauge of program success. Some families may leave services early because they have achieved their goals. In fact, there is surprisingly little evidence that the intended length or actual length of a program is associated with client outcomes.6 It is unclear why this is the case, but it may be partly because families begin to benefit within the first few visits. The Durham Connects model illustrates this point.
- Durham Connects
Durham Connects is a brief model that consists of 4 to 7 in-person or telephone contacts. Results from a randomized trial show that, compared to a control group, families that received Durham Connects had significantly higher scores in positive parenting behavior, home environment quality, and fewer emergency room visits.7 - STEP 1: Birthing visit
The Durham model begins during a birthing hospital visit when a family can schedule up to 3 home visits with the nurse that occur between 3 and 8 weeks of infant age. - STEP 2: Home visits
Visits include information sharing (“teachings”) and assessments for health and psychosocial risk factors. High-risk families are connected to additional community services and maternal and infant health care.
It is also possible that the frequency of visits is as important, if not more so, than the length of services. Research indicates that more frequent visits increase the likelihood of positive outcomes such as increased gestational age8 and enhanced maternal behavior.9 Yet, research also suggests that only about half of families receive the minimum number of recommended visits.10
In response to this challenge, the FFHV program launched a continuous quality improvement (CQI) effort in 2015 to improve the rate of completed home visits. Programs focused on communicating the expectations of visit frequency with families, rescheduling visits immediately, and sharing monthly tracking data with staff. Within nine months of launching the CQI initiative, the percent of families that received at least three-fourths of their expected visits increased from 59% to over 70% of families.
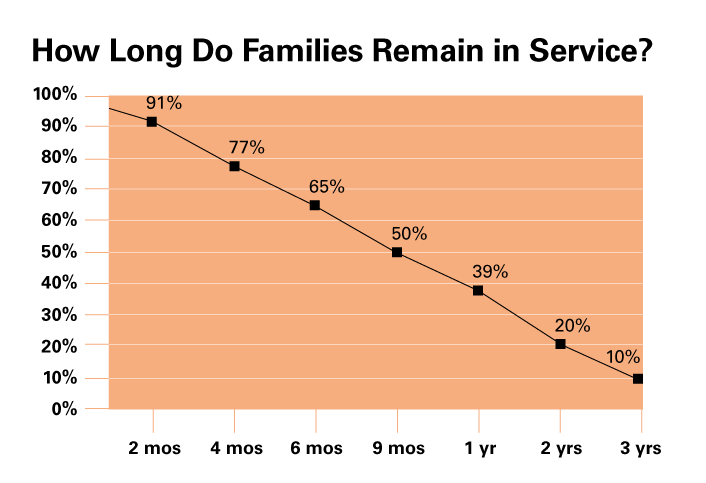
Half of clients that enroll in an FFHV program exit services within the first nine months. These rates are consistent with studies of other home visiting programs.
Engaging Families
Sustained participation is linked to, but also distinct from, family engagement. Engagement is a dynamic, interpersonal process that changes based on interactions between clients and home visitors over time. One concept that captures this evolving relationship is called therapeutic alliance.
Therapeutic alliance refers to the strength of the bond between a client and service provider as well as their agreement on goals and tasks. The FFHV evaluation team developed a brief measure of therapeutic alliance, the Brief Alliance Assessment (BAA), which is designed to match the strengths-based and family-focused orientation of home visiting. Client and home visitor reports are gathered separately and compared to assess their agreement.
Early results from the BAA indicate that both client and staff perceptions of alliance are overwhelmingly positive. For instance, one indicator of mutual bond is trust. Preliminary results indicate that 94% of clients and 88% of home visitors either agreed or strongly agreed that they trusted each other. Goal and task alignment also appears strong, as 96% of clients and 88% of staff report agreement or strong agreement on “what we should focus on when we meet.” Interestingly, compared to staff, clients reported higher average ratings of alliance. This may be a good sign. It could reflect that home visitors need to maintain appropriate professional boundaries. It is also possible that home visitors may have an even stronger connection with families than they realize.
References
1 Kendrick, D., et al. (2000). Does home visiting improve parenting and the quality of the home environment? Archives of Disease in Childhood, 82, 443-451.
2 Gomby, D. S., Culross, P. L., & Behrman, R. E. (1999). Home visiting: Recent program evaluations: Analysis and recommendations. The Future of Children, 4-26.
3 Korfmacher, J., et al. (2008, August). Parent involvement in early childhood home visiting. In Child & Youth Care Forum (Vol. 37, No. 4, pp. 171-196). Springer US.
4 Staudt, M. (2007). Treatment engagement with caregivers of at-risk children: Gaps in
research and conceptualization. J of Child & Family Studies, 16, 183-196.
5 Daro, D. A., & Harding, K. A. (1999). Healthy Families America: Using research to enhance practice. The Future of Children, 152-176.
6 Sweet, M. A., & Appelbaum, M. I. (2004). Is home visiting an effective strategy? Child Development, 75, 1435-1456.
7 Dodge, K., et al. (2014). Implementation and randomized controlled trial evaluation of universal postnatal nurse home visiting. Am J of Public Health, 104, S136-S143.
8 Goyal, N., et al. (2013). Dosage effect of prenatal home visiting on pregnancy outcomes in at-risk, first-time mothers. Pediatrics, 132 (Supplement 2), S118-S125.
9 Nievar, M. A., Van Egeren, L. A., & Pollard, S. (2010). A meta-analysis of home visiting programs. Infant Mental Health Journal, 31, 499-520.
10 Duggan, A., et al. (2000). Hawaii’s healthy start program of home visiting for at-risk families. Pediatrics, 105 (Supplement 2), 250-259.

8 Factors that Influence Participation and Engagement
Motivation
The perceived benefit of services and initial motivation to enroll are key predictors of participation. Clients with lower levels of initial interest are less likely to sustain participation.
Specific Needs
Families of infants with health risks (e.g., low birth weight) are more likely to express interest, enroll, and remain in services.
Family Instability
Frequent moves, intermittent phone service, and family crises can cause families to miss services or leave the program entirely.
Employment
Although half of primary caregivers living below the poverty line in the U.S. are employed, home visiting clients who work receive less visits and are enrolled in services for shorter periods of time than unemployed clients.
Early Outreach
Recruiting families early in pregnancy may increase the likelihood of enrolling and sustaining services.
Staff Characteristics
Home visitors with more experience and lower caseloads have lower rates of client dropouts.
Staff Turnover
Families are more likely to drop out of services early if their home visitor leaves.
Supervision
Frequent, high-quality supervision may promote staff retention and help home visitors improve case planning and services.

