At UWM’s College of Health Professions & Sciences, preparing future healthcare professionals means more than developing expertise within a single discipline; it means learning how to collaborate across them.
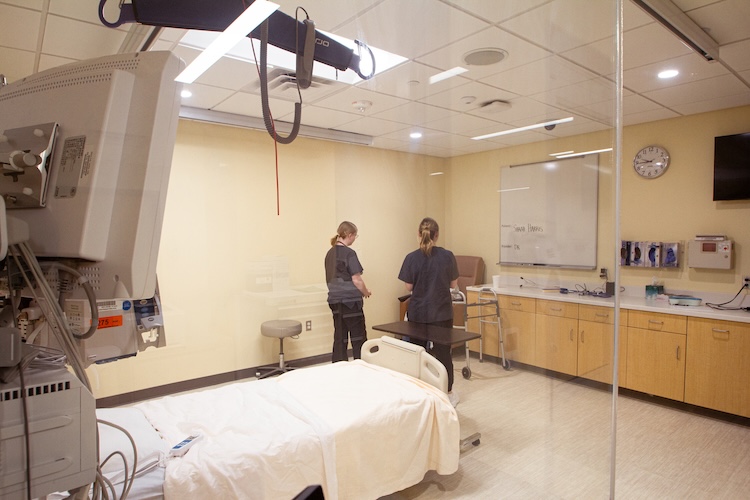
As part of a growing effort within the College of Health Professions and Sciences (CHPS), students from nursing, physical therapy, occupational therapy, and speech-language pathology recently came together for an interprofessional education (IPE) simulation. Hosted in the James and Yvonne Ziemer Clinical Simulation Center, the experience brought learners into a realistic ICU scenario centered on caring for a patient recovering from a stroke.
While IPE has long been incorporated within individual programs, this experience reflects a broader initiative to expand interprofessional simulation across CHPS, creating more opportunities for students to learn with, from, and about one another in meaningful, hands-on ways.
Why Interprofessional Education Matters
In today’s healthcare environment, effective patient care depends on teamwork. Complex conditions like stroke require coordinated expertise from multiple disciplines, each contributing a unique lens to improve outcomes.
IPE simulations are designed to mirror this reality. By working through patient scenarios as a team, students strengthen communication skills, gain a clearer understanding of each profession’s role, and learn how collaborative decision-making leads to safer, more effective care.
The Ziemer Clinical Simulation Center provides an ideal setting for this work. With high-fidelity technology and thoughtfully designed clinical scenarios, students are able to engage in immersive learning experiences that build both clinical confidence and teamwork skills in a safe, supportive environment.
Inside the Simulation
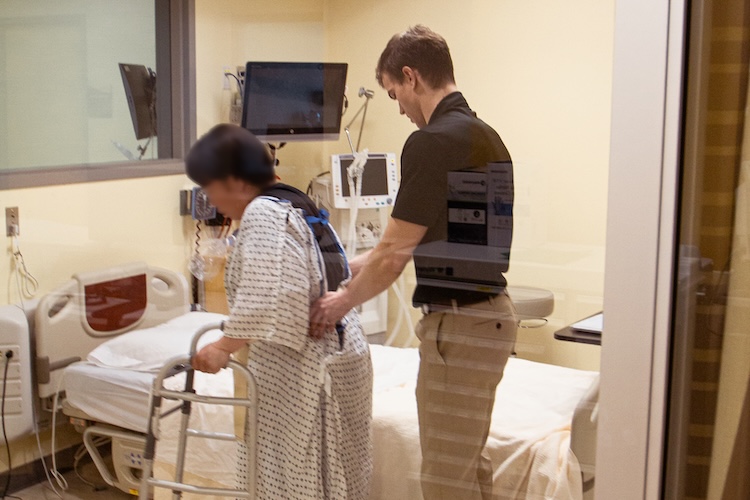
During the simulation, students assessed and managed a stroke patient in the ICU, navigating both the clinical complexities and the interpersonal dynamics of team-based care. Each discipline brought its expertise to the table:
- Nursing students focused on patient monitoring, medication management, and overall care coordination
- Physical and occupational therapy students evaluated mobility, function, and rehabilitation needs
- Speech-language pathology students assessed communication and swallowing concerns
Following the simulation, students participated in a structured debrief, an essential component of simulation-based learning, where they reflected on their decisions, discussed team dynamics, and explored alternative approaches.
Student Reflections
For many students, the experience offered valuable insight into how collaborative care unfolds in practice.
Ryan, a physical therapy student, shared:
“This IPE experience provided more knowledge on the different professions and how they work together. Having a better understanding and application of this teamwork allows me to be more comfortable to use them as resources.”
Lauren, also studying physical therapy, highlighted how the experience prepared her for upcoming clinical work:
“This experience was very beneficial, because as a PT student, I have not had a lot of experience working with other professions. I start an acute care clinical rotation at Mayo Clinic in the summer, and this simulation helped me to gain a better understanding on what it looks like to work with both nursing and speech in patient care. I liked being able to reflect and discuss after the simulation was over, because everyone had various perspectives and different ideas which were helpful to hear.”
For Sarah, a speech-language pathology student, the simulation provided valuable real-world context:
“This IPE simulation felt valuable to my learning, because it gave me insight as to what a real world case might look like in a hospital setting. I do not have much medical experience with speech so to see how I can use my profession to work together in a team that included PTs and nurses was extremely helpful and will allow me to build my skills.”
Alex, a Master of Nursing student, emphasized the broader impact on understanding patient care:
“This simulation helped me better understand how different healthcare disciplines work together to carry out a patient’s care plan. It’s easy to not see the other sides of the care plan when only focusing on your own discipline. This simulation brought all the disciplines to light.”
Dr. Jessica Rotier, Director of Clinical Simulation Education and Research, noted the impact on student learning and the future of care:
“I am incredibly impressed by our students. Their ability to represent their professions, learn from one another, and collaborate so effectively shows how they are changing the culture of healthcare by breaking down silos and working together to provide better patient-centered care.”
Looking Ahead
This simulation is part of a broader effort to expand interprofessional learning opportunities across CHPS. By intentionally integrating IPE into college-level programming, UWM is creating more consistent, meaningful experiences that prepare students for the collaborative nature of modern healthcare.
As these efforts continue to grow, students will graduate not only with strong clinical skills, but with the ability to communicate, collaborate, and lead within interprofessional teams; ultimately improving outcomes for the patients and communities they serve.